Six years after the global rollout of COVID-19 vaccines, stories like the one featured in the headline of lives allegedly “ruined” by vaccine side effects continue to circulate and provoke strong reactions. These accounts raise important questions about vaccine safety, transparency, and how society supports those who experience rare adverse outcomes. But they also sit within a broader scientific and public health context that must be carefully examined.
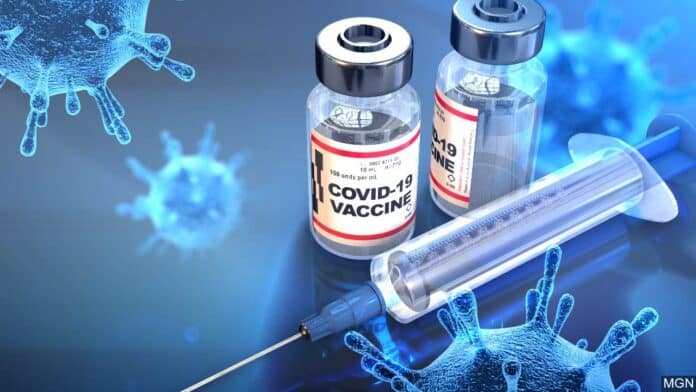
During the pandemic, vaccines such as the AstraZeneca COVID-19 vaccine, alongside mRNA vaccines, were deployed at unprecedented speed. Clinical trials and subsequent real-world data consistently showed that these vaccines dramatically reduced the risk of severe illness, hospitalisation, and death from COVID-19. In the UK alone, health authorities estimate that tens of thousands of lives were saved during the height of the pandemic due to vaccination programmes.
However, no medical intervention is without risk. A relatively small number of individuals experienced serious side effects. One of the most widely documented was a rare condition known as vaccine-induced immune thrombotic thrombocytopenia (VITT), linked in rare cases to the AstraZeneca vaccine. This condition involves unusual blood clotting combined with low platelet counts and, in some instances, proved fatal or life-altering.
Cases like Nikola Brindley’s, referenced in the image below,

reflect the human cost behind these statistics. Individuals who believe they have suffered severe side effects often describe a sudden and profound change in their quality of life, ranging from chronic illness to disability. For them, the issue is not abstract risk but lived reality. Some campaigners argue that their experiences have been minimised or overlooked in the broader public narrative, which overwhelmingly emphasised vaccine benefits.
There is evidence that, in the early stages of the rollout, communication around risk evolved rapidly. Initial messaging focused heavily on urgency and collective protection, which some critics argue left insufficient space for nuanced discussion of rare adverse events. As more data emerged, regulators such as the UK’s Medicines and Healthcare Products Regulatory Agency (MHRA) updated guidance, including age-specific recommendations for certain vaccines.
Yet the scale of risk remains a crucial part of the picture. Studies have consistently shown that serious side effects from COVID-19 vaccines are extremely rare, often measured in a handful of cases per million doses. By contrast, COVID-19 itself carries a far higher risk of complications, including blood clots, organ damage, and long-term illness such as Long COVID. This risk-benefit balance is central to public health decision-making.
That said, rarity does not diminish the responsibility to care for those affected. One area of growing scrutiny is how governments support individuals who experience vaccine-related harm. In the UK, the Vaccine Damage Payment Scheme (VDPS) offers a one-off payment to those who meet strict criteria, including proving severe disablement. Critics argue that the threshold is too high, the process too slow, and the compensation insufficient for lifelong conditions.
Medical professionals also face challenges in diagnosing and managing these cases. Some symptoms reported by patients, such as fatigue, neurological issues, or autoimmune responses, can be complex and difficult to attribute definitively to vaccination. This creates tension between patients seeking recognition and clinicians adhering to evidence-based standards of causation.
The media plays a powerful role in shaping public perception. Headlines that emphasise dramatic individual stories can raise awareness but may also risk distorting the overall picture if not carefully contextualised. Sensational framing can fuel vaccine hesitancy, particularly when readers are not presented with the statistical rarity of such outcomes or the overwhelming benefits observed at the population level.
Conversely, dismissing or ignoring adverse experiences can erode trust. A balanced approach requires acknowledging both truths: that vaccines have been one of the most effective tools in controlling the pandemic and that a small number of people have suffered serious consequences that deserve recognition, research, and support.
Ongoing studies continue to monitor vaccine safety and long-term outcomes. Importantly, the rapid development of COVID-19 vaccines has also accelerated advances in pharmacovigilance, the systems used to detect and analyse side effects. These improvements may benefit future vaccination programmes and medical treatments more broadly.
Public confidence ultimately depends on transparency. Clear communication about risks, however small, combined with visible support for those affected, is essential. This includes funding for research into rare side effects, streamlined compensation systems, and open dialogue between health authorities and the public.
The legacy of COVID-19 vaccination is complex. It is a story of scientific achievement on an extraordinary scale, but also one that includes individuals who feel left behind by that success. Understanding both perspectives is key to building a more resilient and trustworthy healthcare system.
As the world reflects on the pandemic years, the challenge is not to choose between recognising harm and celebrating success, but to hold both in view.