The United Kingdom is facing a quiet but profound public health crisis, one that cannot be dismissed as a statistical anomaly or blamed solely on individual lifestyle choices. New research showing a decline in healthy life expectancy (HLE) should serve as a serious warning: people are not just living shorter, healthy lives; they are spending more years in poor health and the gap between rich and poor is widening at an alarming rate.
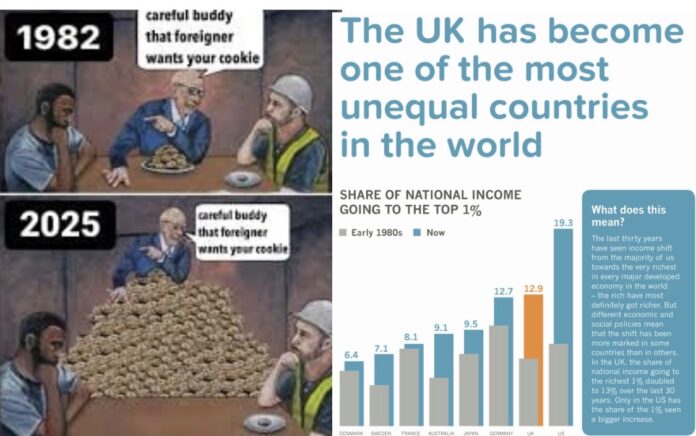
Over the past decade, healthy life expectancy in the UK has fallen by around two years, now sitting at just under 61 for both men and women. Among comparable wealthy nations, the UK ranks near the bottom, an extraordinary fall for a country with vast resources and a longstanding public healthcare system. This is not a marginal shift; it represents a systemic failure affecting millions.
It is tempting, and not entirely wrong, to point to austerity as a central cause. The wave of spending cuts introduced after the 2008 financial crisis reduced funding for local authorities, public health initiatives and social care. These cuts disproportionately affected the most deprived communities, weakening the very systems designed to support health and wellbeing. When services are stripped back, early interventions disappear and preventable conditions become chronic ones.
However, to attribute the decline entirely to austerity would be too narrow an explanation. The UK has long struggled with structural health challenges, including high rates of obesity and chronic illness. These issues did not begin in the past fifteen years, though they have certainly worsened within it. Similarly, mental health, particularly among younger people, has deteriorated significantly, a trend that was sharply accelerated by the COVID-19 pandemic.
What emerges is a more complex picture: austerity did not create these problems, but it intensified them. It reduced the resilience of communities already under pressure and widened existing inequalities.
Nowhere is this more evident than in the stark regional disparities across the country. In affluent areas, people can expect to enjoy decades more of good health compared to those in deprived regions. This is not simply about income; it reflects differences in housing quality, employment opportunities, access to services and environmental conditions. Coastal and post-industrial towns, in particular, have been left behind economically for decades, creating conditions where poor health outcomes are almost inevitable.
The consequences extend far beyond individual suffering. A decline in healthy life expectancy has serious economic implications. Increasing numbers of people are being forced out of the workforce due to ill health, while younger generations face barriers to entering employment or education. When the majority of areas report healthy life expectancy below the state pension age, it exposes a fundamental mismatch between policy assumptions and lived reality.
This is not sustainable. A workforce burdened by ill health cannot support long-term economic growth, nor can it sustain the pressures placed on healthcare and welfare systems.
Addressing this crisis requires more than short-term fixes or political point-scoring. It demands a sustained commitment to tackling the root causes of poor health. Prevention must become a priority, with investment in public health, early intervention and community-based care. Poverty must be addressed not as a side issue but as a central determinant of health outcomes. Housing policy must confront the reality that poor living conditions directly contribute to illness. And regional inequality must be tackled through meaningful economic investment, not slogans or privatisation.

Equally important is a renewed focus on mental health, particularly among younger people navigating an increasingly uncertain economic and social landscape.
The decline in healthy life expectancy is not inevitable. It is the result of choices: economic and social. Reversing it will require different choices, made with a clear understanding that health is shaped long before anyone enters a hospital.
Ultimately, this is about more than how long people live. It is about how well they live and whether the UK is prepared to confront the conditions that are quietly eroding that fundamental measure of a healthy society.